
McConnell’s Ravage Eye Turned Pale Blue. The brown iris of Janice McConnell’s ravaged left eye has turned pale blue. The vision in Gina Macchia’s right eye, with its grossly enlarged pupil, is limited to light and shadows. Both women underwent eye-saving, cornea-transplant surgery this year. They lost months away from their jobs, wear sunglasses to avoid […]
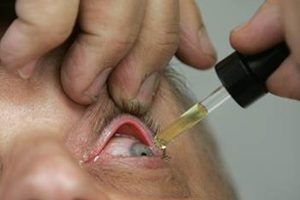
McConnell’s Ravage Eye Turned Pale Blue. The brown iris of Janice McConnell’s ravaged left eye has turned pale blue. The vision in Gina Macchia’s right eye, with its grossly enlarged pupil, is limited to light and shadows.
Both women underwent eye-saving, cornea-transplant surgery this year. They lost months away from their jobs, wear sunglasses to avoid stares and battle a toxic mix of anger, fatigue and frustration.
“Some days I get a little down, but I cope with it. I hang on to some hope that I’m going to see again out of that eye,” said McConnell, 57, a job-program coordinator in Frazer, Pa.
The culprit, a fungal infection so rare that most eye doctors had never seen a case, sent a cold shiver through contact lens wearers around the world. Hundreds of people said they contracted the dangerous microbe while using a new multipurpose lens solution made by Rochester-based Bausch & Lomb Inc.
Consumer lawsuits against Bausch & Lomb have been piling up in U.S. courts, and the debacle could drag down the optical products company’s finances for years. Lawyers now expect 500 to 700 people will seek damages for Fusarium keratitis infections in trials beginning as early as next summer.
Lawsuits could wind up costing Bausch & Lomb $1 billion in damages, analyst David Maris of Banc of America Securities estimated. Losing its dominance in the lucrative lens care market 34 million Americans wear contact lenses could prove even more draining.
Already beset by accounting irregularities at its Asian subsidiaries, the company slashed its 2006 profit forecast by 78 percent. Its share of U.S. lens care kits plunged from 31 percent to 8 percent before rebounding to 21 percent in the July-September quarter, according to Health Products Research in Whitehouse, N.J.
Of the 180 infection victims confirmed so far in 35 states, 59 needed cornea transplants, the Centers for Disease Control and Prevention in Atlanta said. At least 120 more lens wearers were stricken with the infection in the fall of 2005 in Hong Kong, Singapore, Malaysia and China, health officials and lawyers in those countries reported. It later appeared in the U.S.
Several people allege the MoistureLoc solution caused them to lose an eye.
“There were days that I thought I was going insane,” said Macchia, 49, a financial broker’s assistant in Jackson, Mich.
Questions abound over whether Bausch & Lomb reacted quickly enough.
The company stopped selling MoistureLoc in Hong Kong and Singapore in February but only halted U.S. shipments in April. It permanently withdrew the $100-million-a-year product from all markets in mid-May when the Food and Drug Administration called it the “potential root cause.”
After months of testing, the company determined that MoistureLoc’s unique disinfectant and moisture-retention agents, in combination with poor hygiene habits, could in some cases create a thin film that sheltered the fungus from the solution’s sterilizer.
An analysis by leading eye doctors and the CDC concluded that MoistureLoc was the only cleaner implicated, noting the spike in infections rapidly subsided after its worldwide recall.
In the company’s view, spokeswoman Barbara Kelley said, the outbreak was caused by various factors including the ingredients in the solution and how the patients used it.
“The issue is, what is that unique combination of factors that led some people to get the infection and others not?” Kelley said.
While Bausch & Lomb said it acted swiftly to unlock a bewildering medical riddle, the timeline is the crux of the legal battle, said Carl Tobias, a law professor at the University of Richmond in Virginia who specializes in product liability disputes.
“What did they know, when did they know it, and did they move quickly enough once they had information that would lead them to believe people were being hurt by the product?” Tobias asked.
McConnell bought a bottle of MoistureLoc in September 2005, thinking its touted moisturizers might solve the drying of her eyes in wintertime. She was at work in mid-November when she suddenly felt a searing pain as if “a piece of sharp glass” was caught under her lens.
The eye turned beet red. She couldn’t stand the light. She stayed home with the curtains drawn for nearly two weeks, taking antibiotic drops hourly. The pain got so severe, she was rushed to Wills Eye Hospital in nearby Philadelphia and finally diagnosed with the fungal infection.
By January, “the fungus had broken through the cornea, started eating the eye,” McConnell said in a trembling voice. “They dug deep into the eye to get it out.”
The invasive transplant surgery created a blinding cataract that was eventually removed in August. But with her vision deteriorating again, she recently found out she’ll need a new cornea implant. As for the scarred iris, she said, “I’m at the point, I don’t ever care if it turns brown again.”
Robbed of depth perception, McConnell drives only on familiar roads but not at night because “headlights are doubled.” She’s embarrassed by her clumsiness. “I bump into people because I can’t focus,” she said.
In one case, an Oklahoma teenager whose eye infection disseminated through her bloodstream almost died, said Dr. Arthur Epstein, chairman of the American Optometric Association’s contact lens and cornea section. “Some of these patients were terrifically harmed,” he said.
In addition, said the CDC’s medical epidemiologist, Dr. Benjamin Park, “there were some cases that were so severe that they did require” removal of the eye.
Macchia’s attorney, Jason Mark of Parker & Waichman in Great Neck, N.Y., said one client in West Virginia “has to wear a prosthetic shell in her socket because her eye became so deformed from the treatment.”
Macchia’s cornea operation in March lasted 6 1/2 hours.
The doctors “Roto-Rootered my retina,” she said, laughing grimly. “If I keep this cornea, the doctor will fit me with a contact lens as a cosmetic so it’ll look like my other eye. That’ll probably help. Like I told him, I’ll wear anything as long as it’s not Bausch & Lomb.”
The personal injury attorneys at Parker Waichman LLP offer free, no-obligation case evaluations. For more information, fill out our online contact form or call 1-800-YOURLAWYER (1-800-968-7529).


