
Patient Died After A Series Of Blood Centers Human And Computer Errors. A hospital patient died last fall after a series of human and computer errors allowed her to receive a lethal transfusion of contaminated platelets from the Community Blood Center. An instrument used to detect dangerous bacteria had discovered the problem more than 24 hours […]
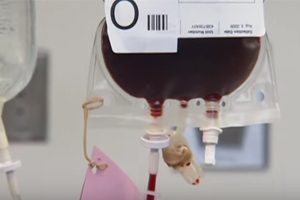
Patient Died After A Series Of Blood Centers Human And Computer Errors. A hospital patient died last fall after a series of human and computer errors allowed her to receive a lethal transfusion of contaminated platelets from the Community Blood Center.
An instrument used to detect dangerous bacteria had discovered the problem more than 24 hours before the patient received the platelets, but the blood center didn’t get the message until it was too late.
The instrument’s warning system has multiple safeguards to ensure that tainted blood never leaves the building. But the alarm never got through for three reasons, according to federal regulators:
The E. coli-laced platelets were delivered to the University of Kansas Hospital on Nov. 21 and given to a leukemia patient. Within 48 hours she was dead.
The blood center is being scrutinized by the Food and Drug Administration, which has found problems with operating procedures, staff training and record keeping.
“I clearly regret every bit of this,” said Jay Menitove, the center’s executive director. “We changed policy. We changed procedure. We changed personnel so this never happens again.”
The FDA and the manufacturer of the detection equipment also issued an alert to blood banks that computer errors may keep warnings from reaching their laboratory computers.
The blood center plays a vital role in health care in the region. It supplies almost all the blood products used by Kansas City area hospitals, as well as scores of hospitals from Topeka to Columbia.
Rich Pendleton, director of the compliance branch of FDA’s Kansas City district office, declined Thursday to comment on the incident.
“Until they can satisfy us they are in compliance, it’s an open case,” he said.
However, the FDA’s findings “shouldn’t be a reflection on their blood supply as a whole,” Pendleton said.
The manufacturer of the detection equipment, bioMérieux, said in a written statement that its BacT/ALERT 3D instrument used by the blood center “accurately identified the blood product as contaminated. The contaminated blood product was unfortunately released by the blood bank.”
The BacT/ALERT system, which is manufactured in St. Louis, is installed in 85 percent of the blood banks in the United States, bioMérieux said.
Both bioMérieux and the FDA issued safety alerts in December warning that the system may fail to report blood contamination to a blood bank’s laboratory computers when there are errors in stored data.
The manufacturer also advised blood banks to leave the audible alarm on and have laboratory personnel check the BacT/ALERT’s control screen at least once per shift.
That should have been obvious to blood banks, said Sidney Wolfe, director of Public Citizen’s Health Research Group, a patient safety advocacy organization based in Washington, D.C.
“It shouldn’t take a letter from the company to tell blood banks not to rely on PCs that can crash,” Wolfe said. “It’s less than clever of a blood bank to turn the alarm off.”
Menitove said the blood center’s staff now leave the alarm on and routinely monitor the control screen.
“We thought we had a system that was better than an alarm system,” Menitove said. “I do believe it was a good system. I thought it was the most robust system. I thought it was a system that could not be shut down.”
However, the system relied on the computer link to the detection instrument.
“Their (bioMérieux) PC screwed up,” Menitove said.
BioMérieux did not respond to Menitove’s statement.
Platelets are the component of blood responsible for creating clots to arrest bleeding. They are often critically needed by cancer patients whose illness or treatment diminishes their supply.
Blood safety experts call bacterial contamination of platelets the most common risk of infection from transfusions.
About one in 1,000 to 3,000 units of platelets each year is tainted with bacteria, causing illness in many patients, according to the Centers for Disease Control and Prevention.
Roughly seven or eight patients die each year from blood infections caused by contaminated platelets.
“Everyone agrees there’s some level of problem, that it’s something we need to focus on,” said Kathleen Sazama, former president of the American Association of Blood Banks.
Unlike donated red blood cells that blood banks keep refrigerated, or plasma, which is frozen, platelets must be kept at room temperature.
That creates an ideal breeding ground for bacteria.
“The bacteria are given a pretty good incentive to grow,” said Sazama, who now is conducting research on platelet safety issues at the University of Texas’ M.D. Anderson Cancer Center.
Two years ago, the national association required blood banks to have methods in place to limit and detect bacterial contamination of platelets. While several devices like the BacT/ALERT system are available, blood banks are still trying to determine the most effective way to detect contamination, Sazama said.
“There are a lot of platelets that are being discarded,” she said. “But it’s a fragile system.”
Platelets can become contaminated when the needle used to draw blood from a donor punctures the skin and picks up bacteria on the surface. In other cases, donors may have bacteria in their blood in amounts too small to make them ill.
Menitove said that when the contaminated platelets were collected on Nov. 18, a Friday, the donor appeared to be in good health.
“The donor had no symptoms whatsoever,” Menitove said, “so my assessment is there is no way of knowing” how the platelets became contaminated.
At 2:54 a.m. that Sunday, the BacT/ALERT system detected bacteria in the platelets.
But when blood center personnel reported to work the following morning, the detection system alarm was off and no one immediately checked the system’s control screen, FDA investigators said in an inspection report.
At 6:06 a.m. that Monday, the platelets were shipped to the University of Kansas Hospital.
A few hours later, the patient received the platelets. She quickly fell ill.
Suspecting a problem with the platelets, the hospital conducted its own tests and found “a significant presence of bacteria in what should be a sterile product,” a hospital spokesman said in a written statement to The Kansas City Star.
“I was notified (of the contamination) sometime before noon by (blood center) lab people,” Menitove said. “They took care of the computer problem.”
At 11:38 a.m., the blood center called the hospital and tried to quarantine or recall the platelets. It wasn’t until nearly an hour later that the center told the hospital the actual reason why it wanted the platelets back, FDA investigators said in their report.
E. coli bacteria are fast-growing and potentially deadly because they produce a toxin, Sazama said.
“It’s very clear even healthy people would have trouble with a bolus of E. coli,” she said. “It just overwhelms everything in the body.”
Menitove said he met with members of the patient’s family within hours after she died.
“I told them what happened and clearly apologized,” he said. “I never want to have to do that again.”
After the patient died, FDA investigators spent much of November, December and January at the blood center.
Among the concerns they raised:
In March, the FDA sent the blood center a letter warning that “to date, your response does not provide assurance to our office that you have taken effective measures necessary to prevent recurrence of the deviations.”
“That’s a problem generally with blood banks; the response is isolated to the symptoms,” said Wolfe of Public Citizen. “They don’t take care of the fundamental problems.”
But Menitove said the center had hired more laboratory staff, given staff more thorough training and changed record-keeping procedures.
When the blood center proposed further corrective actions, the FDA said in April that it had no objections to them.
Another inspection will be needed, however, to confirm compliance with regulations, the agency said.
“It shouldn’t have happened,” Menitove said of the patient’s death. “It shouldn’t happen again.”
The personal injury attorneys at Parker Waichman LLP offer free, no-obligation case evaluations. For more information, fill out our online contact form or call 1-800-YOURLAWYER (1-800-968-7529).


