
Another study has made a connection between Type 2 diabetes drugs known as incretin mimetics and increased rates of developing pancreatitis, a known precursor to pancreatic cancer. Incretin mimetics, are GLP-1-based diabetes therapies and include Byetta and Bydureon (exenatide); Victoza (liraglutide); Januvia, Janumet, Janumet XR, and Juvisync (sitagliptin); Onglyza and Kombiglyze XR (saxagliptin); Nesina, Kazano, […]
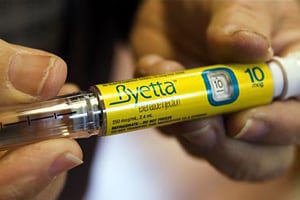 Another study has made a connection between Type 2 diabetes drugs known as incretin mimetics and increased rates of developing pancreatitis, a known precursor to pancreatic cancer.
Another study has made a connection between Type 2 diabetes drugs known as incretin mimetics and increased rates of developing pancreatitis, a known precursor to pancreatic cancer.
Incretin mimetics, are GLP-1-based diabetes therapies and include Byetta and Bydureon (exenatide); Victoza (liraglutide); Januvia, Janumet, Janumet XR, and Juvisync (sitagliptin); Onglyza and Kombiglyze XR (saxagliptin); Nesina, Kazano, and Oseni (alogliptin); and Tradjenta and Jentadueto (linagliptin). Incretin mimetics are made with natural substances that lower raised blood sugar levels and are used in patients diagnosed with abnormally low insulin levels or patients whose bodies do not utilize insulin efficiently. These drugs imitate the body’s incretin hormones, which stimulate the release of insulin following meal consumption.
Bydureon, Byetta, Janumet, Januvia, Jentadueto, Kombiglyze XR, Nesina, Onglyza, Tradjenta, Victoza were reviewed for this study, which examined adverse drug reaction reports (ADRs), according to Italian researchers who confirmed the ties between the drugs and pancreatic damage, AdverseEvents reported. The study results were published in the November 13, 2013 issue of Informa Healthcare.
Earlier this year, the U.S. Food and Drug Administration (FDA) issued a Drug Safety Communication indicating that it was “…investigating reports of possible increased risk of pancreatitis and pre-cancerous findings of the pancreas from incretin mimetic drugs for type 2 diabetes.” The FDA has not yet concluded if regulatory action concerning incretin mimetics should or should not be put in place.
This study reviewed data from the Italian Spontaneous ADR Reporting Database and identified relevant cases of ADRs tied to incretin mimetics. The research team reviewed 1,169 reports involving incretin mimetics, which included 90 cases of pancreatitis or elevated pancreatic enzyme levels, according to AdverseEvents. The researchers concluded that the data demonstrated the connection between incretin mimetics and pancreatic impairment. The researchers also found that patients taking incretin mimetics should be monitored for potential pancreas harm.
Using FDA Adverse Event Reporting System (FAERS) data from November 1, 1997 to December 31, 2012 that was aggregated and standardized by the AdverseEvent RxFilter process, the researchers identified 4,512 reports of pancreatitis and 14 cases of elevated pancreatic enzyme levels in which incretin mimetics were listed as the primary suspect. Of these, the team identified 2,478 hospitalizations and 113 patient deaths in which incretin mimetics were indicated as the primary suspect.
Another published piece in the journal, BMJ, revealed that incretin mimetics might be riskier than first thought. The report also indicated that drug makers have withheld data on the potentially dangerous effects of incretin mimetics. After analyzing thousands of pages of regulatory documents obtained under Freedom of Information rules, BMJ located unpublished data indicating that “unwanted proliferative or inflammatory pancreatic effects,” are associated with use of incretin mimetics.
A study published March 22, 2013 in the journal, Diabetes, revealed abnormal changes, such as precancerous lesions, in the pancreases of eight people who had taken GLP-1-based medications, when compared with patients who took other diabetes medications, according to Medscape Medical News.


