
A cataract surgery left a woman dead after her drug allergy information was ignored. Although the woman’s drug allergy information was noted in medical documents and was also indicated on two medical alert bracelets, Carol Whiteford, 68, died following routine surgery to remove her cataract and implant her with an intraocular lens, according to TheWest.com. […]
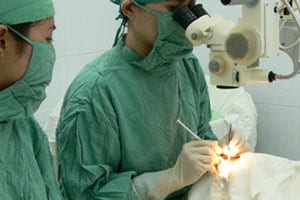 A cataract surgery left a woman dead after her drug allergy information was ignored.
A cataract surgery left a woman dead after her drug allergy information was ignored.
Although the woman’s drug allergy information was noted in medical documents and was also indicated on two medical alert bracelets, Carol Whiteford, 68, died following routine surgery to remove her cataract and implant her with an intraocular lens, according to TheWest.com. An inquest into her death revealed that Whiteford died a few hours after her surgery and that her death was the result of an allergic reaction to a prescription medication. She died on March 6, 2008.
Whiteford was suffering from shortness of breath and was sweating heavily within 10-15 minutes after a nurse at Northam Hospital treated her with a sulphur-based drug. The drug had been prescribed by Whiteford’s eye surgeon, Dr, Andrew Stewart, according to TheWest.com to minimize post-operative blood pressure spikes. Her condition rapidly deteriorated; she died as her physicians were preparing to air-lift Whiteford to another hospital, wrote TheWest.com.
According to inquest data, some 14 documents were in Whiteford’s file that indicated she was allergic to sulphur-based drugs. Whiteford was also wearing a red alert bracelet given to patients with allergies. Whiteford met with Dr. Stewart in September 2007; however, there was no information recorded in her file about her allergies or adverse drug reactions, according to the inquest. Dr. Stewart said it was part of his typical routine to ask patients considering surgery about prior drug reactions or allergies.
Dr. Stewart also said that had he been told of Whiteford’s allergies, he would have recorded that in her information. The coroner plans on investigating if the doctor made an error or if an oversight was involved, TheWest.com reported. A review of how Whiteford’s allergy information was recorded at the hospital will also be reviewed to determine if hospital policy and guidelines were appropriately, accurately, and adequately followed.
The registered nurse—Rebecca Nind—who treated Whiteford with the drug Dr. Stewart prescribed said she was unaware the drug contained sulphur and that she would have assumed the medication was safe for Whiteford given that her physician prescribed the drug and should have been aware of her allergies, TheWest.com wrote.
Hospital errors have been in the headlines in recent months. In one case, a surgeon at New York City’s Mount Sinai Medical Center was relieved of administrative and clinical duties after removing the wrong kidney from a patient on dialysis with two failed, diseased kidneys, according to the Associated Press (AP). In 2008, a Minneapolis surgeon removed the wrong kidney from a cancer patient, according to the AP. A state investigation revealed that the operating surgeon was distracted by pager calls and misread the patient’s chart.
Prior to that, a medical error at Kings County Hospital in New York left a single mother from Brooklyn, New York with less than one year to live.
Esmin Green, 49, died at Kings County Hospital Center (KCHC) after writhing on the floor of its psychiatric emergency ward for a full hour. She was in the ward waiting area for over 24 hours before she began convulsing, collapsed, and died due to blood clots caused by a long period of physical inactivity. Surveillance footage revealed that Green appeared to be ignored and unattended while hospital workers and other patients in the room did nothing. In addition to staff repeatedly ignoring Green, patient records were falsified.


