
Research presented at the meeting of the American Urological Association suggests an association between the volume of robot-assisted prostate surgery at a hospital and complication rates for the procedures. Hospitals with the fewest robot-assisted radical prostatectomy (RARP) procedures had a 14.7% complication rate, while complications occurred in about 5.7% of cases at the highest-volume hospitals, […]
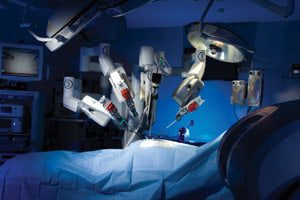
Study Links between Robotic Prostate Surgery & Complications
Research presented at the meeting of the American Urological Association suggests an association between the volume of robot-assisted prostate surgery at a hospital and complication rates for the procedures.
Hospitals with the fewest robot-assisted radical prostatectomy (RARP) procedures had a 14.7% complication rate, while complications occurred in about 5.7% of cases at the highest-volume hospitals, MedPage Today reports.
Jesse Sammon, DO, of the Henry Ford Health System in Detroit, reported that these findings suggest that market and reimbursement forces created a “perverse disincentive” that discourages hospitals with a low volume of RARP procedures from referring patients to high-volume centers. “As more institutions acquire a robot,” Sammon said, “in the U.S., the fee-for-service model tends to disincentivize referral to high-volume institutions.” Once a facility has invested in a surgical robot, the institution has an incentive to promote its use, even for as few as 25 to 30 cases a year. Sammon feels this may jeopardize patient care, according to MedPage Today.
The co-chair of the meeting session, Dr. Christopher Kane, of the University of California San Diego, noted that Sammon and his colleagues previously reported data showing that the safety of open radical prostatectomy has declined in recent years, and this coincided with a sharp decline in the volume of all open surgical procedures. “Could it be that high-volume surgeons are migrating to RARP, so that the only people doing open radical prostatectomy are the low-volume surgeons operating at relatively low-volume hospitals?” Kane asked.
Sammon acknowledged that men living in large metropolitan areas still have access to high-quality open prostate surgery. “f you’re living in the suburbs, it doesn’t make any sense to go to the guy down the street who is doing 25 robots a year.” But access to quality open radical prostatectomy is not certain, even in cities. Fewer hospitals offer open prostatectomy and fewer surgeons are now training in open techniques, according to MedPage Today.
Kane said Sammon’s data suggest that over time RARP has become safer and open radical prostatectomy has become “slightly less safe.” Dr. Eric Klein of the Cleveland Clinic said a crucial factor in the decision is the physician’s experience. “No matter how you do it, experience counts, and that’s what data show.” Klein noted that about a decade ago in Britain health regulators mandated that major pelvic procedures be performed only at centers with an annual volume of at least 50 cases of the procedure in question.
Sammon said RARP was rapidly adopted throughout the U.S., and by 2008 was the dominant form of radical prostatectomy. But, he said, the rapid spread of robotic technology occurred in the absence of level 1 (randomized clinical trial) data and with limited observational data for RARP, according to MedPage Today.
A comparison of outcomes by procedural volume suggested, “f you were going to get a low-volume radical prostatectomy procedure, you were probably better off at an open radical prostatectomy center,” according to Sammon. Data for 2009 to 2011 showed 802 hospitals offered RARP in 2009, 792 in 2010, and 808 in 2011. Complication rates had a direct association with volume, increasing from 5.7% for very-high-volume centers to 8.8% for high-volume, 9.8% for intermediate-volume, 12.2% for low-volume, and 14.7% for very-low-volume, MedPage Today reports.


