Study Finds Endoscopes Not Properly Cleaned at Medical Facilities
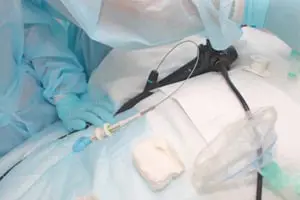
According to an online article by Reuters, a recent study indicated that medical facilities are not adequately cleaning their endoscopes before reuse on other patients. This improper cleaning can lead to cross-contamination and severe infections. Experts are now recommending alternative practices in an effort to prevent infections and improve patient safety during endoscopy procedures.
Current Guidelines Allow for Reuse of Endoscopes
Endoscopies allow physicians to view areas of patients’ bodies using a long, flexible tube with a light and camera on the end. The camera will produce images of the relevant area of the body, and the physician can then analyze those images to develop an appropriate treatment plan for the patient.
Current guidelines by the Centers for Disease Control and Prevention allow for reuse of flexible endoscope tubes when healthcare facilities “reprocess” or clean the equipment. Reprocessing is supposed to involve thorough cleaning, full sterilization, complete drying, and proper storage before the endoscope can be used on another patient. If facilities implement these practices, the CDC allows for reuse of endoscopes between patients.
However, new studies show that reprocessing procedures might not be adequate to protect patients. Many healthcare facilities do not follow the CDC guidelines, and even health care facilities that do follow all the guidelines can end up with contaminated endoscopes. Contaminated endoscopes present a severe risk of infection when used on subsequent patients.
Studies Show Reprocessing Not Eliminating Infection Risks
A newly published American Journal of Infection Control study evaluated the reprocessing practices of three multispecialty hospitals. Researchers examined endoscopes at these facilities used for various types of endoscopy procedures, including upper gastrointestinal endoscopies, lower gastrointestinal endoscopies, and urological endoscopies, among others. They found that two of the facilities were skipping significant steps or performing the steps poorly, and the third facility used appropriate practices. However, all three facilities failed tests for contaminated endoscopes.
The study found that the risks for contamination were highest in reusable bronchoscopes and urology scopes. Researchers in the study found indicators of organic contamination in 22 percent of the endoscopes they studied, with 71 percent containing microbial growth. Twenty-two of the 45 endoscopes they examined contained leftover fluid. None of the drying methods used by the facilities resulted in complete fluid elimination, even where proper procedures were followed. Also, all of the facilities were using some damaged endoscopes.
Following results of the study, epidemiologists have emphasized the importance of ensuring that guidelines are always correctly implemented and that endoscopes are completely dry before facilities store them away. Fluid residue presents a significant risk of cross-contamination and infection, they say, because patients come into contact with bodily fluids from other patients and growing bacteria.
In concluding the study, the researchers found that current reprocessing and storage guidelines are not safe and effective, even when fully implemented. They recommended facilities begin to use sterilized endoscopes or at minimum perform regular audits and clinician inspections to ensure patient safety.
FDA Critical of Certain Endoscope Equipment
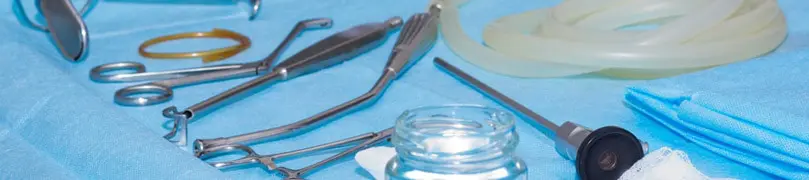
The above study is not the only criticism endoscope equipment, and practices have faced lately. The U.S. Food and Drug Administration recently advised against the use of certain gastrointestinal endoscope connectors because of the risk of cross-contamination.
On April 18, 2018, the FDA released correspondence in which it advised health care providers against using 24-hour multi-patient use endoscope connectors for gastrointestinal endoscopies. The FDA said these specific connectors expose patients to potential cross-contamination because they do not have indications for reprocessing or backflow prevention features.
Endoscope connectors are cap-like components used to connect endoscope tubes with irrigation equipment. Irrigation allows physicians to introduce water from a bottle that will flow through a water channel and clean the endoscope camera. Physicians sometimes favor irrigation because it will enable them to wash away mucosa and keep the camera picture clear. Connectors join the water bottle to the endoscope. Some of these connectors are single-use (used on only one patient during one procedure), and some are multi-use (used during multiple procedures on different patients).
Most multi-use connectors come with instructions and guidance for reprocessing, but a subset of connectors — 24-hour multi-patient connectors — are marketed for use with multiple patients without the need for reprocessing. These connectors also do not have backflow prevention features, which stop patient fluid from traveling back into the endoscope. The FDA believes these specific connectors are unsafe and should not be used in endoscopy practice.
In its April 18 letter, the FDA advised against the use of 24-hour multi-patient connectors, like the ERBEFLO port connector, manufactured by Erbe USA Inc. The FDA made the following recommendations to health care providers:
- Do not use 24-hour multi-patient endoscope connectors because they carry a risk of cross-contamination.
- Use single-use endoscope connectors with backflow prevention features; or
- Use reusable/multi-use (not 24-hour multi-patient) connectors with backflow prevention features, and ensure the connectors are adequately reprocessed before each use.
Cross-contamination presents a severe risk to patients. Patients who undergo endoscopies with contaminated endoscopes can develop severe infections that require extensive medical treatment, hospitalization, and surgeries. Medical experts and the FDA are working to spread awareness and encourage facilities to follow guidelines in place and implement internal checks to make sure they maintain patient safety.
Reporting Contamination to the FDA
Patients who develop infections following endoscopy procedures can report their experiences to the FDA by using the agency’s Adverse Event Reporting System. This system allows both patients and health care providers to notify the FDA of health issues with a particular procedure, device, drug, or treatment. Patients can provide a significant amount of detail, and the FDA will review their submissions.
When the FDA notices a significant number of adverse events related to the same product or matter, it will evaluate whether it needs to release safety communication or take further action regarding warnings, training, label changes, etc. The FDA’s safety communication regarding 24-hour multi-patient endoscope connectors was in part prompted by reports of adverse events and infections sent to the agency through its Adverse Event Reporting System.
Additional information about the FDA’s Adverse Event Reporting System can be found on the FDA’s website.
Parker Waichman LLP: Experienced Medical Negligence and Device Lawyers
Parker Waichman LLP has extensive experience litigating medical negligence and medical device cases. We offer free case consultations and perform full-scale reviews of all potential claims to provide our clients with options for moving forward. We understand when our clients are dealing with serious injuries, they need timely answers to their case questions, and we always strive to maintain superior client communication.
Our law firm has secured more than $2 billion in settlements and verdicts for victims and families, and we approach every personal injury case with the same dedication to justice. If you have potential medical negligence or medical device claim, including a claim regarding an infection following an endoscopy, contact our offices today to discuss your case details with an experienced attorney. We litigate cases around the country and can help you achieve the results you need.
Contact Parker Waichman LLP today by calling 1-800-YOURLAWYER (1-800-968-7529) or by filling out the Contact Form on our website.








